- Providing Health Solutions Nationwide

Our integrated healthcare plan solution works in a seamless fashion with our service-first program partners.
Our concierge team serves as the center of the healthcare universe to a member, and it begins with HELLO! Our multi-lingual care team will call at the beginning of the plan year to introduce themselves to the members to build a relationship, and they will guide the member through every healthcare episode that they encounter.
The concierge team will verify if the member’s provider participates in the network and if not, they will contact the provider to negotiate an agreement allowing the member to continue seeing the provider.
Our concierge team will be the single source of contact for every member.

Join us in creating a brighter, healthier future by embracing strong partnerships to redefine wellness and success.
FGI works with a Third-Party Administrator that has over 29 years of experience in the healthcare industry. We are uniquely aligned with a service-first approach to our clients. The TPA is the owner of the source code and employees over 49 IT programming professionals. This ensures their operating system and team members serve the client in the most efficient and precise manner.

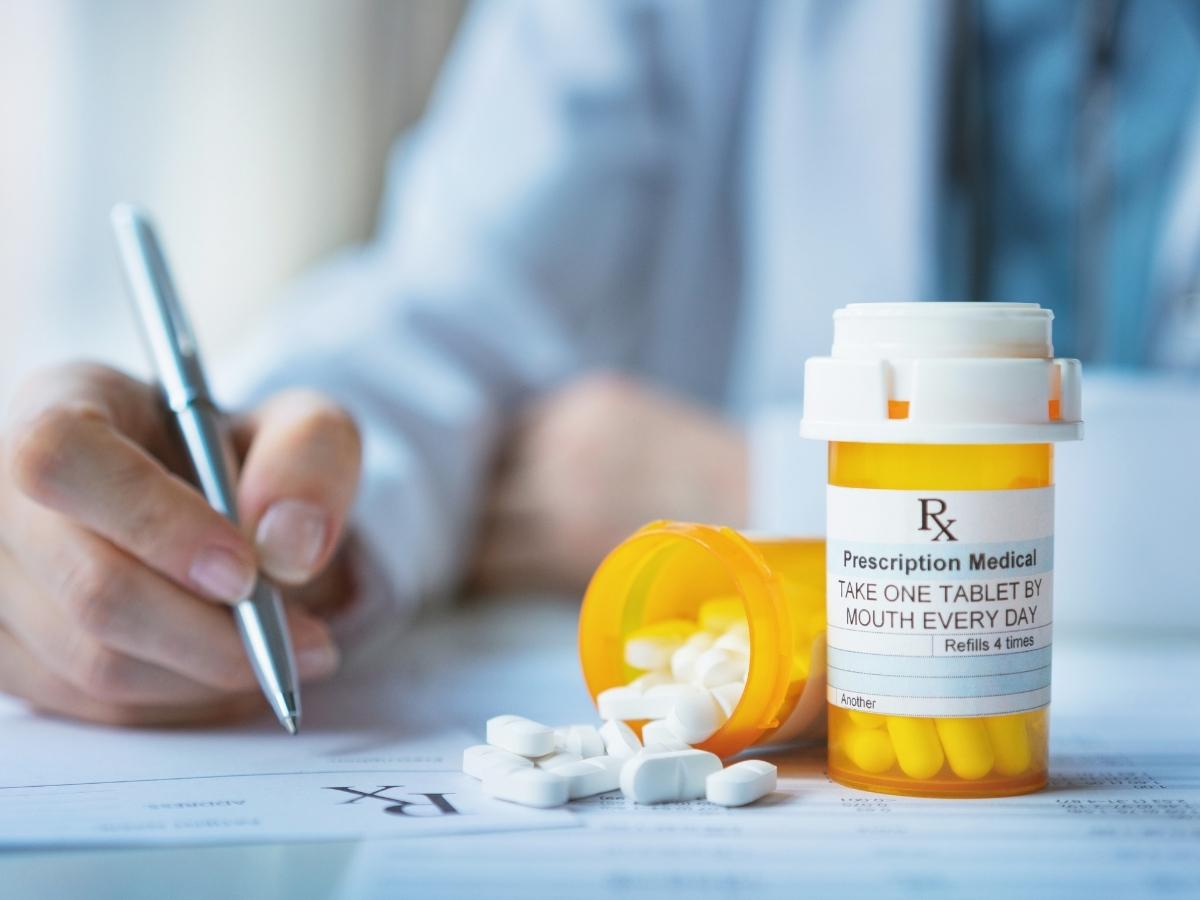
The unsustainable cost of prescription drugs is having a negative impact on the healthcare system. Prescription spending is growing faster than any other part of the healthcare dollar and prescription expenditures represent 30%-40% of the total healthcare spend. Over the past 10 years, prescription medications has risen 3x faster than the rate of inflation and prescription drug costs have increased in the U.S. by 35% in the past 5 years.
We have partnered with an innovative, tech-driven prescription benefits organization that focuses on lowering costs. While most PBMs talk about cost transparency, our program prefers to be cost transparent and innovative by utilizing state-of-the-art technology combined with human intervention to create real savings and value. Our strategic approach of utilizing mail order for maintenance medications, International Pharmacy, Prescription Assistance Programs (PAP) and others will have a dramatic impact in controlling the overall pharmacy spend on a healthcare plan.

We offer a full suite of URAC-accredited services (Utilization Management, Case Management, and Disease Management) to improve access and target the most appropriate levels of care before services are rendered, resulting in dramatic savings for the plan and the member. Our partner has the ability to be proactive instead of reactive in delivering quality healthcare at the best possible price.
Through our program partners, we have the ability to provide in-depth reports identifying trends in healthcare spending as well as specific opportunities to improve the level of care and cost avoidance on a member level.
Our reporting provides guidance for evaluating the performance of the health plan which allows us to analyze benefit structure, areas of cost prevention, and clinical intervention.


FGI has preferred MGUs / Stop Loss Carriers that have fully analyzed our program and our seamless approach to providing services on an efficient platform in combination with sound cost containment strategies to provide the most competitive pricing for stop loss coverage.
In addition to traditional experience underwriting, we have the ability to underwriter utilizing AI technology on groups with 10 or more enrolled employees without needing individual health questionnaires or experience. This option is great for groups wanting to move from fully insured or coming out of an association or PEO plans with no experience.


Our program includes comprehensive virtual healthcare with a leading telemedicine company that provides medical care at a $0 copay, and no claims cost to the plan.
It also provides behavioral health services that include copays to the member and no claims cost to the plan.
Making decisions for one’s health is not just an administrative function; it is a personal experience. That is why we offer a best-in-class platform that not just saves clients’ time, stress, and money – it supports every step towards better health benefits usage and engagement.
This all-in-one benefits app unifies member experience by having everything in one place: ID cards, Plan Summaries, Virtual Care, Care Navigation, Provider Lookup, Provider Comparison /Transparency Tools, Pharma, Claims Data. Also includes a member communications tool that sends secure, HIPAA-compliant messaging to groups and individual members to ensure the right message at the right time.

Discover what our satisfied clients have to say about their transformative experiences with The Freshour Group. Real stories, real results – see how we’ve made a difference in their healthcare journeys.
The Freshour Group has transformed the way we approach healthcare benefits. Their integrated solutions have led to significant savings for our clients, and the member experience is exceptional.
"*" indicates required fields